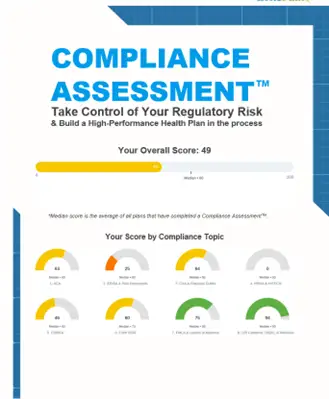
Your Compliance Assessment Tool for Health & Welfare Benefit Plans
BRITEPATH is pleased to be able to provide our clients with this valuable resource in collaboration with Health Rosetta.
It serves as the catalyst in our pursuit to transform a health plan from ‘Pay More, Get Less’ into a High-Performance Health Plan capable of eliminating the hidden costs and artificial prices that plague the status quo health care and insurance ecosystem.
Once you’ve submitted your basic plan information below, BritePath will send you your Compliance Assessment within 3-5 business days.
Instructions
As you fill this form out, there may be questions you don’t know the answer to or are unsure. “No” should be your answer for these (or leave a box unchecked). This process is designed to establish a baseline and you can always return and complete the information again. Even the best plans have areas that need work and/or a benefit hasn’t been well communicated. If you have questions, please email info@britepathbenefits.com.
Please Complete the Form Below:
Compliance Assessment is an in-depth review of your plan’s compliance with applicable federal regulations related to health benefits. Because these regulations are complex and ever-changing, many employers are unknowingly exposed to potential liability for noncompliance. This report evaluates your practices and compliance risk, highlighting any deficiencies and areas for potential improvement. Compliance Assessment will help you cut though the complexity, educate yourself, and provide direction to help you minimize risk.
The federal government has recently created new regulatory requirements and increased employee benefit plan oversight, with a particular focus on topics related to transparency and plan sponsor fiduciary duties under ERISA. Noncompliance is costly and can result in hefty fines and penalties, plus regulators more proactively enforce requirements than in the past. Compliance Assessment will help you identify gaps and provide direction to mitigate risk. It can play a key piece of your overall plan improvement strategy. Highlighting potential compliance issues also helps draw attention to other areas for plan improvement, such as member communications, vendor selection, plan design, etc. For example, improving how you communicate compliance notices to plan members can serve as the starting point for a broader assessment of your overall member communication strategy. Another example is that focusing on improving fiduciary duty compliance requires understanding the strengths and weakness of your vendors, which also supports your broader vendor selection process.
You and your trusted benefits advisor should evaluate Compliance Assessment results to create a plan for improving areas of weakness or noncompliance. You may find that you need or want to partner with an outside organization to help you meet requirements and potentially outsource some risk. Complete the Assessment at least once per year to track your progress and improvement, while quickly learning about new or changed requirements.
While Compliance Assessment provides a comprehensive view of federal regulations that apply to typical health benefits plans offered by private sector employers, you should understand its limitations, where it applies, and where it only partially applies.
- It relies on the accuracy of data you provide, so it is critical to provide correct information.
- It does not cover any state level requirements that may apply, such as those under state departments of insurance.
- It does not provide guidance on whether a plan qualifies for specific exemptions under ERISA that may apply to churches and governmental entities.
- It does not go into detail on certain topics that require additional analysis, such as how to evaluate a group of related companies to determine controlled group analysis. However, it highlights these topics that require deeper assessments to help you define next steps.
- It does not fully cover issues related to unions, VEBA’s, PEO’s, association plans, MEWA’s, or other less common types of plans. These unique circumstances require specialized analysis to determine how various regulations apply.
DISCLOSURE
Please note that Health Rosetta is not a law firm and cannot provider legal advice or certification of regulatory compliance. Nor does Health Rosetta provide tax advice. This document provides an assessment of general compliance risk to your group health plan. We encourage you and the Plan fiduciaries to consult with your legal and/or tax counsel regarding all potential compliance issues identified by Health Rosetta. You agree that this assessment is provided only as a tool and that Health Rosetta has no discretionary authority or control with respect to the management or administration of your employee benefit plan(s).
What is the Health Rosetta?
The Health Rosetta is a blueprint for high-performance health benefits. It is a practical approach built on what successful purchasers do. This is an evolving ecosystem of brokers, advisors, consultants, doctors, attorneys, and a vast network of professionals that are committed to scaling healthcare solutions that have already been validated all over the country.