Do you feel in control of your healthcare costs?
Healthcare costs are rising uncontrollably.
Employer premiums rising far faster than inflation.
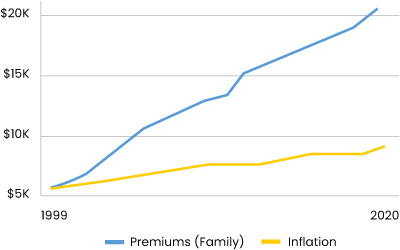
Seem impossible to control...
- Impenetrable and Invisible – no data to make decisions.
- Appears overwhelmingly complex.
- After a bad year, costs go up. After a good year costs stay the same (or go up).
Leading to the "Healthcare Paradox".
"IT IS WHAT IT IS"
Despite healthcare often being the 2nd largest expense after payroll for many employers, it receives little scrutiny while much smaller expenses are closely managed.
WHAT'S THE IMPACT ON YOUR EMPLOYEES?
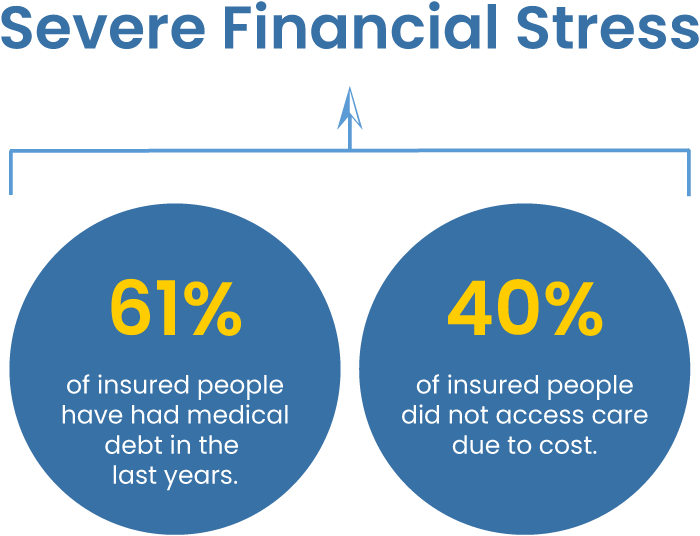
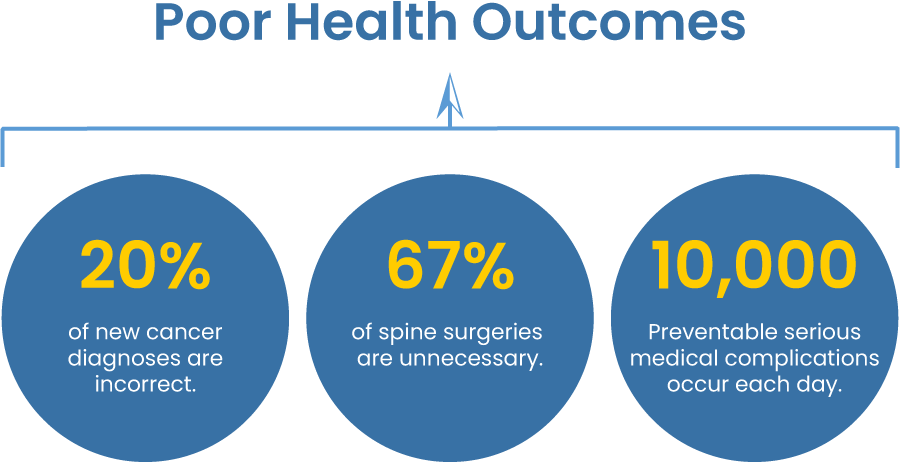
Poor health outcomes and severe financial stress are the norm
Employer Premiums and Deducibles Have Risen Much Faster than Wages Since 2010
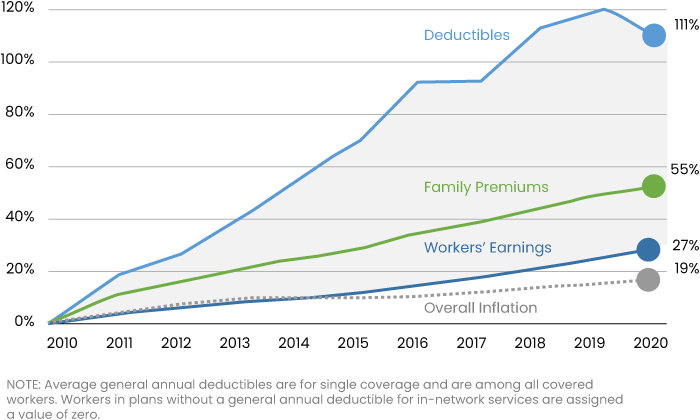
High Premiums and Out-of-pocket costs…
Since 2000, health insurance premiums have risen 272%, employee contributions have increased 202% and out-of-pocket costs now exceed $9,000 for individuals and twice that for families.
WHY DOES THIS PERSIST?
The system is set up to protect the satus quo.

Misaligned incentives: Insurance carriers make money by you spending more on healthcare, not less.

Just the 4 biggest carriers made $11 billion in profit in a single quarter (Q3 2022)

Information about your plan performance is deliberately impenetrable to avoid scrutiny.
CAN THIS BE SOLVED?
The solution exsists: A viable, proven, employer-focused healthcare model.

1
It all begins with the decision to take action.
2
You can make your health benefits benefit you.
The Plan Grader analyses the most important factors and practices of high-performance health plans, creating an independent assessment of the eight Health Rosetta components.
Tackling these eight Health Rosetta components puts plan sponsors in the driver’s seat to improve health outcomes while controlling and reducing costs for the organization and its employees.

Plan Grader™ analyzes the 40 most important factors of high performance health plans, creating an independent health plan assessment across eight Health Rosetta components within LOCAL adoption continuum.
Tackling these eight Health Rosetta components puts plans in the driver’s seat to improve health outcomes while controlling and reducing costs for you and your employees.
The following pages include an in-depth view on each compontent within the overall context of the LOCAL adoption framework.
1
Transparent Advisor Relationships
2
High-Performance Plan Design, Docs, and Risk Mgmt.
3
Independent, Active Plan Management
4
Major Specialities and Outlier Patients
5
Transparent Pharmacy Benefits
6
Individual Stewardship
7
Value Based Primary Care
8
Transparent Open Networks
The results of the Plan GraderTM set the stage that enables a plan sponsor, along with aligned partners, to transform the current underperforming health plan into a high-performance plan.
Your Overall Score: 49

*Median score is the average of all plans that have completed a Plan Grader™.
Your Score by health rosetta component
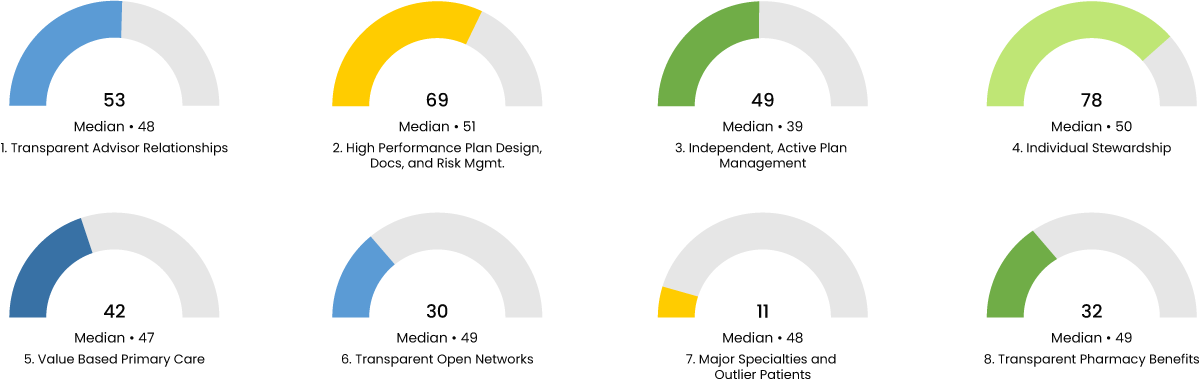
3
Your BritePath Advisor guides you through the transition.
A high-touch customer-service model supports you at each stage.
Strategize
- Gather and analyze available data, contracts, and Plan Grade
- Decide how to quickly make changes.
- Develop a multi-year action plan.
Implement
- Choose vendors and sign contracts
- Create compliance and change management plan.
- Engage and inform all plan members.
- Launch data strategy and analytics.
Optimize
- Regular, comprehensive plan performance reviews.
- Adjust ad extent your multi-year plan.
- Decide how to invest your Health Rosetta Dividend.
4
Your business and employees will be delighted by the new plan.
Is it really worth the effort to make the change?
BENEFITS TO EMPLOYERS
- Healthcare costs that are predictable and budgetable from year to year.
- Opportunity to invest back into your business and employees with monies saved.
- High quality, affordable healthcare that leads to happier, higher performing employees.
- Massive savings: 10-40% annually.
BENEFITS TO EMPLOYEES
- Relieved of financial stress from unsustainable costs.
- Faster, better access to higher quality care.
- Lower stress and less time spent on healthcare.

